This story is free to read because readers choose to support LAist. If you find value in independent local reporting, make a donation to power our newsroom today.
Disneyland Beckoned As A Pandemic Escape, But This Vaccinated Family Still Got COVID

By early July, Disneyland was open with most of its pre-pandemic magic, and hefty lines, intact. Park-goers didn't have to wear masks or keep six feet away from strangers, in accordance with California’s rollback of many mandates in June, when the state reopened.
“It was so overwhelming from a sensory perspective,” says Mike McHargue.
He and his wife, Jenny, along with their two teenage daughters, had chosen this as their first big family outing, a nostalgic reminder of trips when the girls were little, and of a time before COVID-19.
They were excited to spend a few days at the park but seeing thousands of people without masks was jarring. As they stood in line for the Peter Pan ride, they discussed the likelihood of coming in contact with an infected person.
“Mike even [mentioned] that first day... the probability of people walking in the park that had COVID," Jenny recalls. "And [those] that had the actual Delta variant."
The couple had carefully chosen the dates of their trip, waiting until both their teenage daughters were fully vaccinated.

“I wanted to beat the inevitable rise in cases that would come with reopening, to minimize our chances, even as vaccinated people. There wasn't a lot of case spread in the community yet. On paper it worked," Mike says.
They wore masks on the trip but the night they drove home to La Crescenta, Jenny felt ill. She didn’t think much of it until a couple of days later, when her sense of smell disappeared.
“She opened the jar of garlic to see if she could smell it. She said, ‘I think I can smell this.’ And it almost knocked me over on the other side of the room. And I said, ‘I'm going to go get us COVID tests right now,'" Mike says.
Despite being fully vaccinated, both Mike and Jenny tested positive for COVID-19.
“I did start crying because it was like, we did everything right. And now, what, we have to be in another kind of forced lockdown, just when we had this little bit of freedom?” Jenny says.
Weeks later, their younger daughter tested positive.
Cases Go Up As Masks Come Off
Less than two weeks after California’s reopening lifted almost all coronavirus restrictions, including a public mask mandate, cases began to climb. By the time the McHargues went to Disneyland in early July, new COVID-19 cases and test positivity rates had more than doubled in L.A. County.
On July 1, county health officials were raising the alarm.
“Given that we have large numbers of unvaccinated people in Los Angeles County, four million in total, including 1.3 million children not yet eligible to be vaccinated, another wave could become a very real possibility,” said Barbara Ferrer, director of the County Public Health Department at a press briefing.
Despite warnings of the threat of the highly transmissible Delta variant, and recommendations to wear a mask indoors ahead of the Fourth of July holiday weekend, more people contracted the virus. Case numbers surged to levels not seen since last February.
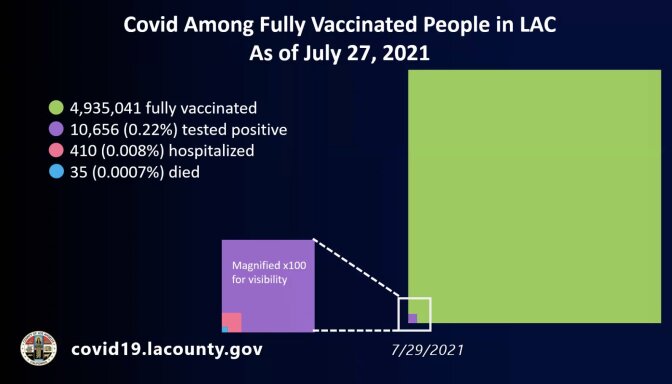
Alongside the huge increase came an unsettling fact: a quarter of the people in L.A. County testing positive in the first two weeks of July were vaccinated.
More Breakthroughs Due To Delta
“If it hadn't been for Delta, we wouldn't be in this situation,” says Eric Topol, a physician and molecular medicine professor at Scripps Research in La Jolla. “The real issue is that we don't know the transmission rate [between vaccinated people] but we do know it’s happening.”
The Delta variant, Topol says, is more dangerous. It has a shorter incubation period, of just four days, making people contagious sooner. It also tends to produce more of the virus inside people's bodies. That means some vaccinated people will transmit the virus to others.

“Obviously, it's going to be low because most vaccinated people are not going to get infected. And even those who do get infected are going to be automatically asymptomatic and only detected through testing,” he adds.
Topol says it’s impossible to predict exactly how Delta will behave in the future but watching countries such as India provides some clues. Delta virus outbreaks tend to last 10 to 12 weeks.
“We have to face it and it's going to be circulating for several weeks. And during that time, wearing a mask indoors, especially, is important,” Topol says.
Topol applauds L.A. County health officials for being among the first in the nation to reinstate an indoor mask mandate for everyone, regardless of vaccination status. “L.A. County was smart to do that,” he says.
But California’s statewide mask mandate remains a thing of the past. It was scrapped in June, when cases were low. That’s when millions of people, including live entertainment producer Nina Storm, headed out to reopened restaurants and comedy clubs.
“If I was doing something social and fun, I didn't wear a mask inside,” she recalls.
After a quick getaway in Palm Springs, she suddenly experienced intense body aches, heavy congestion and fatigue. She tested positive the next day.
“What I've gone through is basically like having a bad flu, which isn't the end of the world as much as it's not been fun,” Storm says.
She’s recovering at home with over-the-counter medications but has never doubted her decision to get vaccinated: “Absolutely, stand by it, 100%. Had I not been vaccinated, it could be much worse, much longer, much more extreme, much scarier.”
Only a tiny fraction of vaccinated people end up in the hospital due to COVID-19 but some vaccinated people do have more serious cases.
If I Get COVID, How Much Will It Cost?
A few days after they returned from Disneyland, Jenny McHargue convinced her husband to go to the emergency room. He was having trouble breathing.
“By that evening, he was like, ‘Yeah, I think it’s best for me to go,’” Jenny says.
Mike’s chest was X-rayed to check for blood clots, a side effect that hadn’t occurred to them. The medical team didn’t find any and Mike was eager to check out as soon as his blood oxygen improved. He wanted to keep his hospital costs down.
It has taken a few weeks but his cough and constant fatigue are slowly getting better. Mike uses his asthma inhaler to help treat his coughing fits. Now, he has other worries.
“I'm terrified of when the bill comes,” he confesses. “You're literally saying, Do I want potentially life saving medical intervention at the cost of, truly debilitating medical debt? It's a terrible situation.”

Under federal law, health insurance companies are not required to cover the full cost of COVID treatment, only diagnostic testing and related services such as office visits. During the height of the pandemic, some insurers chose not to charge COVID patients, and a few have continued that policy as long as the public health emergency is in place. But many companies have quietly reverted to business as usual.
Mike is wary of medical bills after a cardiac event in 2019 almost wiped them out financially. They are only solvent due to an online fundraiser that raised more than $50,000 towards the cost of care.
“We have really expensive health insurance that somehow manages to never pay for anything,” he says.
Now, with the threat of more medical bills hanging over their heads, they may have to again ask friends and family for financial help.
“I don't want to try to do another GoFundMe,” he says. “But who knows what's going to come in the mail."







